WHAT IS OSTEOPOROSIS?
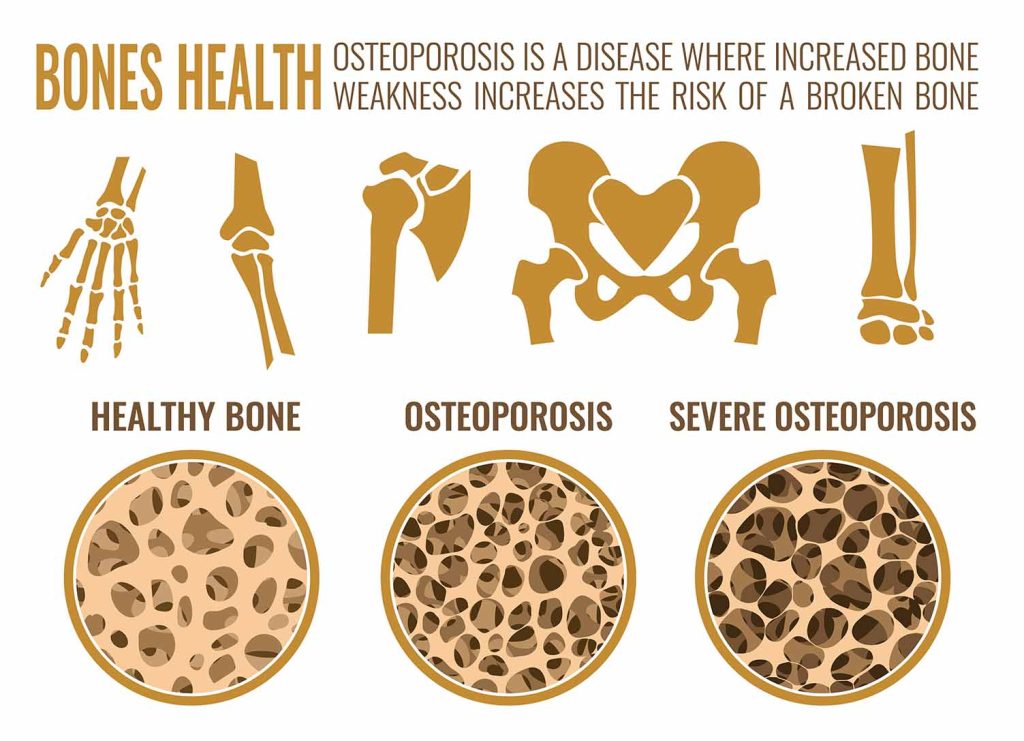
Osteoporosis is a common and well-defined disease that affects millions of people worldwide. It is characterised by a loss of bone mineral density and bone strength, which can lead to fractures and other serious health problems.
WHAT CAUSES OSTEOPOROSIS?
The skeleton is a metabolically active system, constantly being remodelled throughout our lives. Osteoblasts are cells that signal the body to build bones, while osteoclasts instruct the body to break down bone and release stored minerals like calcium into the bloodstream.
When these two signalling molecules are coordinated, we have healthy and strong bones. However, when there is a disruption in the communication between these cells, bone is destroyed faster than it is produced.
This process is controlled by the parathyroid gland, which sends a message to osteoclasts to chew up bone and release calcium into the bloodstream.
RISK FACTORS FOR OSTEOPOROSIS
Bone density is at its highest during early adulthood until the late 20s and gradually decreases from around the age of 35. This process is regulated by various factors including cytokines, hormones, nutrition and growth factors.
Women are at a higher risk of osteoporosis due to hormonal changes during menopause which affect bone density, particularly the loss of oestrogen.
For men, the cause of osteoporosis is unknown, but low levels of testosterone have been linked to an increased risk. Although men continue producing testosterone into old age, those with low levels are at a greater risk of developing osteoporosis.
Causes of poor bone quality and osteoporosis include:
- Ageing
- Being female
- Hormonal factors – decline in oestrogen and progesterone (women) and testosterone (men)
- Diet high in refined carbohydrates
- Vitamin and mineral deficiencies (vitamin D, calcium, magnesium, boron, trace minerals)
- Some medications (e.g., steroids)
- Gut issues (nutrient malabsorption)
- Family history of osteoporosis
- Low body weight
- Sedentary lifestyle/lack of exercise
- Excessive alcohol intake and smoking
HOW TO PREVENT OSTEOPOROSIS
Although osteoporosis cannot be cured, you can take steps to prevent it and manage the condition if you have it. Prevention should start early in life, before bone health starts declining. Here are some ways to reduce your risk of osteoporosis:
GET PLENTY OF CALCIUM & VITAMIN D
Calcium is essential for strong bones, and vitamin D helps the body absorb calcium. Good sources of calcium include dairy products, leafy greens, and fish. Vitamin D can be obtained through exposure to sunlight or supplements.
REGULAR EXERCISE
Weight-bearing exercises like walking, jogging, and weightlifting can help build and maintain bone density.
QUIT SMOKING & REDUCE ALCOHOL CONSUMPTION
Smoking and excessive alcohol intake can both contribute to bone loss.
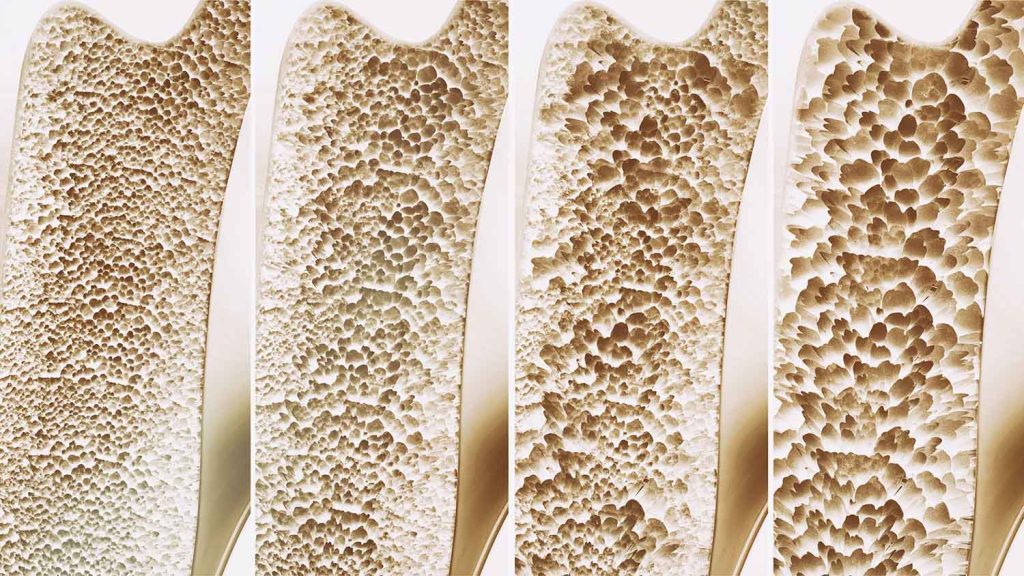
OSTEOPENIA: THE STAGE BEFORE OSTEOPOROSIS
Osteoporosis is often referred to as a ‘silent condition’ because it can develop slowly over the years without any noticeable symptoms until a fracture occurs.
The stage before osteoporosis is known as osteopenia, which is a milder form of bone loss. If detected and treated early, osteopenia can be managed to reduce the risk of developing into osteoporosis later.
HOW TO DETECT OSTEOPOROSIS
BONE DENSITY SCREENINGS
These are done through a dual-energy X-ray absorptiometry (DEXA) and are considered the ‘gold standard’. These machines measure bone density in specific areas of your body including hips, spine, or sometimes your entire body.
URINE AND BLOOD TESTS
There are three bone reabsorption markers (bone resorption is the process by which osteoclasts break down bone tissue:
- N-telopeptide (urine test)
- C-telopeptide (blood test)
- Deoxypyridinoline (urine test).
These three markers fluctuate throughout the day so it’s important to do the tests at the same time each day.
HOW CAN NUTRITION & LIFESTYLE SUPPORT OSTEOPOROSIS?
Osteoporosis can be managed or prevented with the right nutritional and lifestyle changes. A Functional Medicine nutritionist can help identify the underlying cause of symptoms associated with osteoporosis and design a treatment plan to support your bone health. Check out the tips below to get started:
1. EAT A LOW ACID DIET
Maintaining a slightly alkaline pH level in the blood can prevent osteoporosis. Eat plenty of fruits and vegetables (alkaline) to balance animal protein such as red meat, chicken, or fish (acidic) in your diet. Add seeds, nuts, beans, and legumes (if not allergic) for additional sources of protein. Reduce refined foods and consider adding collagen to your diet, which is widely available in supplement form and powders that can be added to smoothies, drinks, and other foods. Bone broth can also be a good source. Avoid alcohol, especially white wine.
2. TAKE VITAMIN D & K SUPPLEMENTS
Due to intensive farming practices, the soil is lacking in minerals, which is one of the reasons why people are more deficient nowadays. Buy organic when possible and take a good quality vitamin and mineral supplement to restore these trace minerals.
Vitamin D is essential for calcium absorption and bone mineralization. Ask your doctor to check your levels at least twice yearly or order a test via Nutrition Diets. Sub-optimal vitamin D status has been reported in many populations, but it is a particular concern in older people.
Vitamin K promotes bone formation, prevents bone resorption, and regulates extracellular matrix mineralization.
Work with a nutritionist to take the right products in the right amounts, and remember it is important to ensure there are no contraindications should you be taking specific medicines for osteoporosis or other health issues.
3. REGULAR EXERCISE
Regular exercise, such as walking, can prevent bone loss and make your bones stronger, reducing the risk of a fracture in the future. Aim to incorporate at least 20-30 minutes of physical activity into your daily routine. Consider yoga and Pilates, which can help with skeletal alignment, very important for healthy bones and hips as well as for balance. A comprehensive exercise program that includes weight-bearing aerobic exercise and stretching is ideal.
4. BALANCE YOUR HORMONES
Oestrogen and Progesterone play an important role in bone metabolism. Speak to your doctor about Biodentical Hormone Replacement Therapy, or consult with a Functional medicine nutritionist and follow a nutrition and lifestyle programme aimed at promoting your hormonal health.
5. LIMIT CAFFEINE AND FIZZY DRINKS
Caffeine increases the rate at which calcium is excreted in urine. Limit your caffeine intake to no more than 2 cups per day and avoid soft drinks as well. In addition to containing caffeine, they are also high in phosphorus, which directly interferes with calcium absorption.
6. AVOID ALCOHOL AND SMOKING
Smoking weakens bones, and women who consume more than 2 alcoholic drinks per day are at the highest risk for osteoporosis.
7. GET QUALITY SLEEP AND REDUCE STRESS
Sleep deprivation can lead to an accumulation of fat in the liver and increase the risk of developing non-alcoholic fatty liver disease (NAFLD). Chronic stress can increase inflammation in the body and contribute to the development of liver disease. It can also cause changes in the gut microbiome, which can impact liver health. Therefore, it’s important to prioritise healthy sleep habits and manage stress as part of a comprehensive approach to liver disease prevention and treatment.
8. CONSUME CALCIUM RICH FOODS
A healthy diet that includes calcium-rich foods is good for bones.

YOUR HEALTH. YOUR CHOICE.
Osteoporosis is a serious condition that can greatly affect your quality of life. However, by understanding the causes and risk factors for osteoporosis, as well as ways to prevent and manage the condition, you can take steps to maintain good bone health throughout your life.
We offer thorough clinical assessment via easy and convenient online consultations and specialise in personalised nutritional therapy, lifestyle solutions and comprehensive Functional testing.
Getting started is simple and free. Take action to optimise your bone health and reduce your risk of osteoporosis.
