Mitochondria, often referred to as the powerhouses of the cell, play a crucial role in your health and ageing process. These tiny organelles are responsible for producing the energy that your cells need to function effectively.
But did you know that mitochondrial health contributes to much more than energy production? It influences metabolism, hormone balance, immune function, brain health, and how resilient the body is as we age.
When mitochondrial function is compromised, the body’s ability to produce and regulate energy declines. Over time, this can contribute to persistent fatigue, brain fog, poor exercise tolerance, slow recovery, mood changes, and signs of accelerated ageing — even when diet and lifestyle appear “healthy” on the surface.
In this month’s comprehensive guide, we explore how your mitochondrial health influences other areas of your health and how you can support your mitochondrial function with at-home testing, targeted nutrition, and evidence-based lifestyle strategies.
The majority of the body’s energy, approximately 90%, is produced by mitochondria in the form of ATP via TCA cycle and the electron transport chain (ETC).
How Do Mitochondria Impact Our Health?
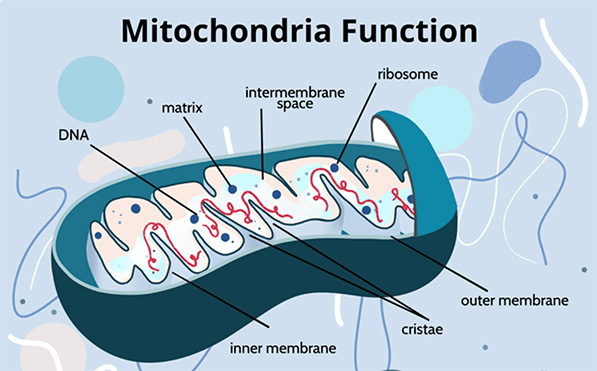
The primary function of mitochondria is to generate adenosine triphosphate (ATP), the main energy currency of the cell, through oxidative phosphorylation. This process, also known as cellular respiration, allows the body to convert nutrients from food into usable energy, supporting the function of almost every tissue and organ.
Beyond energy production, mitochondria play a key role in regulating metabolism, inflammation, cell signalling, and programmed cell death. When mitochondrial function is robust, cells are better able to adapt to stress and maintain optimal function.
Conversely, mitochondrial dysfunction is increasingly associated with chronic health conditions, metabolic disorders, neurodegenerative disease, and accelerated ageing.
How To Recognise Symptoms of Mitochondrial Dysfunction
Many people who become interested in mitochondrial health are not “unwell” in a conventional sense, they simply feel depleted, flat, or not quite themselves. These symptoms are often subtle at first and can be dismissed as stress, ageing, or “just getting older”.
Common signs that mitochondrial function may be under strain include:
- Brain fog or difficulty concentrating
- Digestive symptoms such as bloating or nausea
- Muscle weakness or aches
- Persistent fatigue despite adequate sleep
- Slow recovery from workouts or illness
- Low resilience to stress
From a functional medicine perspective, these symptoms are rarely caused by mitochondria alone. Instead, they often reflect a broader pattern involving nutrient status, gut health, hormone balance, inflammation, stress response, and environmental exposures – all of which influence cellular energy production. This is why addressing mitochondrial health effectively usually requires a whole-body, personalised approach, rather than isolated supplements or lifestyle changes.
👆 If two or more of the above symptoms feel familiar and persist despite lifestyle changes, a free 15- minute personalised Discovery Call can help assess whether you are experiencing mitochondrial stress, and what the next best steps are for your health.
How Do Mitochondria Impact Ageing and Cognitive Decline?
Mitochondrial function naturally declines with age, leading to reduced cellular energy production and increased oxidative stress. During energy production, mitochondria generate reactive oxygen species (ROS) as a by-product. Over time, excess ROS can damage mitochondrial DNA, impairing efficiency and creating a cycle of further oxidative stress.
This process contributes to age-related decline and is linked to conditions such as cardiovascular disease, metabolic dysfunction, and neurodegenerative disorders including Alzheimer’s and Parkinson’s disease.
Because mitochondria sit at the intersection of energy, inflammation, and cellular repair, they are often considered a foundational focus in longevity-oriented nutrition and functional medicine.
How Does Mitochondria Dysfunction Affect Mental Health?
The brain has exceptionally high energy demands, which is why mitochondria are abundant in brain cells. They provide the ATP required for neurotransmitter synthesis, synaptic communication, and neuroplasticity.
Impaired energy production, combined with oxidative stress and inflammation, can disrupt neurotransmitter balance and stress resilience with emerging research linking mitochondrial dysfunction with depression, anxiety, and cognitive decline.
Clinically, this often presents as “wired but tired” patterns such as low energy, reduced mood resilience, poor concentration, particularly when chronic stress, inflammation, nutrient depletion, or sleep disruption are present.
Oxidative stress associated with mitochondrial damage has been postulated to play a role in the pathogenesis of neuropsychiatric disorders, particularly depression and dementia.

How Do Toxins & Environmental Stressors Affect Mitochondrial Function?
Environmental stressors can place a significant burden on mitochondrial health by increasing oxidative stress and disrupting the enzymes involved in cellular energy production. When exposure is chronic, or when detoxification pathways are overwhelmed, this can contribute to reduced energy, poor recovery, and accelerated ageing.
From a functional medicine perspective, the focus is not on fear or elimination of every exposure, but on understanding total load and supporting the body’s ability to process and clear stressors effectively.
Heavy Metals
Metals such as mercury, lead, cadmium, and arsenic can interfere with mitochondrial enzymes and the electron transport chain, reducing ATP production and increasing oxidative damage. Even low-level, long-term exposure can contribute to fatigue, cognitive symptoms, and poor recovery.
Pharmaceuticals
Certain medications, including statins and some antibiotics, have been associated with mitochondrial “collateral damage” by inhibiting pathways involved in energy production (for example, CoQ10 synthesis). This does not mean medications should be stopped, but it can help explain persistent fatigue or muscle symptoms in some individuals.
Chemical Toxins
Pesticides, herbicides, plastics (such as BPA and phthalates), and other industrial chemicals have been shown to impair mitochondrial function and increase oxidative stress. These compounds may also disrupt hormone signalling, indirectly affecting energy regulation.

Book a Free Discovery Call
Discuss your health concerns with one of our expert practitioners and find out how functional medicine can get your health back on track.
How Functional Health Testing Can Support Mitochondrial Health
While lifestyle strategies are essential, many people reach a plateau where symptoms persist despite “doing everything right”. In these cases, functional testing can help identify what is limiting cellular energy production. The appropriate test depends on your individual symptoms but may include:
Targeted nutrient testing can help identify whether deficiencies in nutrients such as vitamin D, B vitamins, magnesium, or methylation-related markers may be limiting cellular energy production.
Rather than supplementing blindly, comprehensive nutrient testing helps clarify whether mitochondrial function is being constrained at a biochemical level; allowing for precise, personalised support.
Chronic stress and disrupted cortisol rhythms can impair mitochondrial recovery and increase fatigue.
The DUTCH Plus test measures daily cortisol patterns to assess whether stress dysregulation may be contributing to low energy, sleep disturbance, or burnout.
This is particularly relevant for individuals experiencing persistent fatigue despite maintaining a healthy lifestyle.
The gut plays a central role in nutrient absorption and inflammation regulation, both critical for mitochondrial performance.
The Comprehensive Stool Test (GI Map) Plus Zonulin assesses microbial balance, pathogens and inflammatory markers, as well as evaluating gut barrier integrity.
If nutrients are not being absorbed effectively, or if chronic inflammation is present, mitochondrial energy production can suffer — even with an excellent diet.
Test. Don’t Guess.
Get the answers you’re looking for with our wide range of at-home health tests. Easy to order. Easy to use.
7 Ways to Improve Mitochondrial Health Naturally: A Functional Medicine Approach
When supporting mitochondrial health from a functional medicine perspective, the goal is to reduce factors that impair energy production while actively supporting the biochemical pathways mitochondria rely on to function efficiently. This typically involves a combination of nutrition, lifestyle adjustments, and where appropriate, personalised assessment to guide targeted support.
1. Optimise Diet and Nutrition for Mitochondrial Energy Production
Mitochondria depend on a steady supply of nutrients to generate ATP efficiently. These nutrients act as cofactors in the Krebs cycle and electron transport chain, directly influencing how much energy cells can produce. Key nutritional considerations include:
- Amino acids: Which support tissue repair and metabolic pathways. Foods include poultry, eggs and dairy, quinoa and tofu.
- B vitamins (B1, B2, B3, B5, B12): Support energy metabolism. Sources include leafy greens, nuts, and seeds.
- Healthy fats: Found in avocados and fatty fish, these provide a stable fuel source for mitochondrial function.
- Iron: Essential for oxygen transport and mitochondrial respiration. Grass-fed red meat is a healthy source of iron.
- Magnesium: Vital for over 300 biochemical reactions, including energy production. Magnesium-rich foods include nuts, seeds, and whole grains.
🔎 Clinical insight: While a nutrient-dense diet is key, many people, even with a healthy diet, experience functional nutrient deficiencies due to gut dysfunction, chronic stress, medication use, or increased metabolic demand. If you are experiencing persistent fatigue or poor recovery, this may signal the need for more personalised and targeted assessment.

2. Use Supplements Strategically to Support Mitochondrial Pathways
Targeted supplement protocols can support mitochondrial function when specific needs or deficiencies are identified. Commonly used supplements in mitochondrial support protocols include:
- Acetyl-L carnitine: Helps transport fatty acids into mitochondria for energy production
- Alpha-lipoic acid: Acts as a potent antioxidant and supports mitochondrial enzymes
- Coenzyme Q10 (CoQ10): Acts as a key component of the electron transport chain
- NAD+: Supports energy production and cellular repair
- PQQ: Promotes mitochondrial biogenesis
Importantly, supplementation should not be generic or excessive. In functional medicine, supplements are carefully selected based on symptoms, health history, and, where appropriate, test findings, to avoid unnecessary cost or metabolic imbalance.

3. Consider Intermittent Fasting Carefully
Intermittent fasting (IF) has been widely studied for its effects on metabolic health and cellular ageing. In appropriate individuals, it may support mitochondrial function by improving energy efficiency and cellular resilience. Potential mitochondrial benefits of intermittent fasting include:
- Boosts Insulin Sensitivity: Improved insulin sensitivity from IF regulates blood sugar levels more effectively, reducing metabolic strain on mitochondria and promoting optimal function.
- Enhances Mitochondrial Biogenesis: IF stimulates mitochondrial biogenesis by activating signalling molecules like PGC-1α and AMPK, which promote the formation of new mitochondria.
- Improves Metabolic Flexibility: During fasting, the body switches from using glucose to fatty acids and ketones for energy, reducing reactive oxygen species (ROS) production. This shift protects mitochondria from oxidative damage and improves their function.
- Increases Production of Key Molecules: Fasting boosts the production of sirtuins, NAD+, and ketones, all of which support mitochondrial function and energy production.
- Promotes Autophagy: This is the body’s process of cleaning out damaged cells and regenerating new ones. This helps remove dysfunctional mitochondria, reducing oxidative stress and maintaining a healthy mitochondrial population.
- Reduces Inflammation & Oxidative Stress: IF lowers systemic inflammation and oxidative stress, creating a more favorable environment for mitochondrial health. This protection helps maintain mitochondrial DNA and protein integrity.
Common approaches include the 16:8 method, the 5:2 method, and alternate-day fasting.
However, IF is not appropriate for everyone. In individuals with chronic stress, hormonal imbalance, a history of disordered eating, pregnancy, or significant fatigue, fasting may increase physiological stress and worsen symptoms.
From a functional medicine perspective, intermittent fasting should be personalised rather than applied as a one-size-fits-all strategy.
4. Support Gut Health to Improve Mitochondrial Function
A healthy gut microbiome significantly supports mitochondrial function. Beneficial gut bacteria produce short-chain fatty acids (SCFAs) like butyrate, which enhance mitochondrial efficiency and biogenesis. A balanced microbiome also regulates inflammation and reduces oxidative stress, protecting mitochondria from damage.
Additionally, a healthy gut improves the absorption of essential nutrients like B vitamins and CoQ10, crucial for mitochondrial energy production.
Following a gut-friendly diet that incorporates probiotics and prebiotics to supports your microbiome enhances mitochondrial function, energy production, and overall well-being.
🔬 Gut health testing is often a foundational step when addressing persistent fatigue, low energy, and poor recovery, even when diet appears adequate. For more information, visit our How It Works page or book a free 15-minute Discovery Call with one of our expert practitioners to discuss your health concerns.
5. Use Exercise to Stimulate — Not Deplete — Mitochondria
Physical activity is one of the most effective ways to stimulate mitochondrial biogenesis, encouraging the body to produce more and healthier mitochondria. Generally supportive forms of movement include:
- Low-intensity aerobic activity such as walking
- Resistance training to preserve muscle mass
- Moderate cardiovascular exercise
However, excessive high-intensity training without adequate recovery can increase oxidative stress and worsen symptoms in individuals with compromised energy systems. When fatigue is persistent, a phased approach that rebuilds capacity while addressing underlying stressors is often more effective than pushing harder.
6. Reduce Toxic Load and Support Detoxification Pathways
Rather than extreme “detoxes”, functional medicine focuses on reducing exposure, supporting the body’s natural detoxification processes, and ensuring adequate nutrient status so mitochondria are not under constant oxidative stress. Simple, practical changes can make a meaningful difference over time.
- Avoid Plastic Containers: Plastics can leach chemicals such as BPA and phthalates into food and drinks, which may interfere with mitochondrial and hormone function. Where possible, use glass, stainless steel, or silicone alternatives.
- Avoid Processed Foods: Processed foods are more likely to contain additives, pesticides, and chemical residues that increase oxidative stress. Choosing whole, minimally processed foods, and organic options when available, can reduce toxic load.
- Consider a Detox Program: Incorporate a short-term detox protocol guided by a healthcare professional to cleanse and reboot your system. Get in touch with us to learn more about our Detox Programme. Short-term detox protocols should always be guided by a qualified practitioner. Extreme or unsupervised “cleanses” can place additional stress on mitochondria rather than support them.
- Filter Your Water: Tap water may contain chlorine, heavy metals, or other contaminants. A good-quality water filter can reduce exposure and support overall cellular health.
- Use Natural Cleaning Products: Many conventional cleaning products contain harsh chemicals that can affect mitochondrial function. Natural alternatives such as vinegar, baking soda, and simple plant-based products are often better tolerated.
7. Prioritise Sleep and Stress Regulation
Sleep is essential for mitochondrial repair and regeneration. During deep sleep, cells repair oxidative damage and restore energy-producing capacity.
Chronic stress, poor sleep quality, blood sugar instability, and cortisol dysregulation often interact to suppress mitochondrial function.
Addressing sleep and stress together, rather than in isolation, is frequently key to restoring energy, resilience, and cognitive clarity.

Key Takeaways
- Mitochondria are central to energy, ageing, and resilience
- Fatigue and brain fog often reflect deeper metabolic or inflammatory stress
- Nutrient status, gut health, stress hormones, and toxic load all influence mitochondrial function
- Lifestyle changes are essential, but not always sufficient
- Personalised functional assessment and health testing can help identify what is limiting energy production and how to support mitochondrial health
Frequently Asked Questions About Mitochondrial Health
What are the most common signs of poor mitochondrial health?
Common signs include persistent fatigue, brain fog, poor exercise tolerance, slow recovery, low stress resilience, and feeling that energy levels are declining faster than expected with age.
Can improving mitochondrial health help with ageing?
Supporting mitochondrial function is considered a key factor in healthy ageing. Efficient energy production helps maintain muscle mass, cognitive function, metabolic health, and overall resilience as we age.
Are supplements necessary to support mitochondrial health?
Not always. Nutrition, sleep, movement, and stress management form the foundation. Supplements may be helpful when specific deficiencies or increased demands are identified, but they are most effective when tailored to the individual rather than taken generically.
How does gut health affect mitochondrial function?
The gut microbiome influences nutrient absorption, inflammation, and metabolic signalling – all of which affect mitochondrial efficiency. Poor gut health can limit energy production even when diet and supplementation are adequate.
When should I consider speaking to a practitioner about low energy or fatigue?
If fatigue, brain fog, or poor recovery persist despite lifestyle changes, a practitioner-led assessment can help identify underlying imbalances and guide a more targeted approach.
YOUR HEALTH. YOUR CHOICE.
Supporting mitochondrial health is one of the most powerful ways to improve long-term energy, resilience, and healthy ageing. A functional medicine approach focuses on identifying and addressing what is limiting cellular energy production in each individual.
If you are experiencing persistent fatigue, poor recovery, or feel that your energy and vitality are not where they should be, a personalised, practitioner-led assessment can help move you from uncertainty to clarity.
At Nutrition Diets, our functional medicine approach considers your unique genetic makeup, diet, environmental exposures, lifestyle factors, and health history:
1) Expert one-to-one therapy
2) Personalised nutrition and lifestyle plans
3) Easy, at-home functional testing
We offer thorough clinical assessment and therapy via convenient online consultations. Getting started is simple and free so why not take charge of your health today with our science-based strategies?



